Introduction

Pelvic Organ Prolapse (P.O.P.) is very common and seen in 43% to 76% of women. This can be seen in young and older women. In younger populations childbirth related, Pelvic floor muscle trauma, this can occur after prolonged and hard labor and giving birth to a “big baby” (more than 9 to 10 lbs). In the older population this can occur due to the stretching out of supportive ligaments.
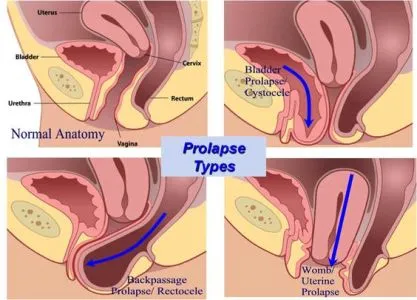
P.O.P. or simply prolapse is the downward descent of the female pelvic organs, (Vagina,Uterus,Bladder and Rectum) .
Prolapse Terminology:
Cystocele or Urethrocele: Bladder prolapse
Rectoclele or Enterocele: Rectum prolapse .Rectal prolapse is not the same as hemorrhoids.
Uterine Prolapse: The vaginal vault prolapse.
Urodynamics: Bladder function test that evaluates urinary incontinence or difficulty urinating.
Cystoscopy: A procedure that uses a camera to look and assess for any anatomical abnormalities that contribute to urinary symptoms.
Defecography: A radiological study that looks at bowel function and prolapse symptoms. .

Risk factors for developing Prolapse:
- The loss of uterine and bladder support, connective tissue lax and weak.Some women are genetically predisposed to lax tissues.
- Chronic constipation.
- Systemic disease, Ehlers-Danlos syndrome
- Chronic coughing
- Obesity
- Menopause
- Heavy lifting and repetitive intense activities such as CrossFit
- Smoking

Degrees of Prolapse:
P.O.P. is said to be of 3 degrees mild , moderate and severe.The degree of prolapse is graded by the organs descent in relation to the hymen.
1. Mild P.O.P. : Most women are asymptomatic , no complaints of symptoms are expressed until the organ be it uterus , bladder or rectum has prolapsed past the hymen.
- In mild P.O.P. loss of this support results in urethral hypermobility and cystocele(bladder prolapse) which is thought to cause stress urinary incontinence (DeLancy 1994) hence these 2 ( ie bladder prolapse and stress incontinence) usually coexist especially with mild prolapse.
2. Severe P.O.P. : symptoms include vaginal bulge that can be seen and felt, and can be the uterus, bladder or rectum that can be causing it.
- Urinary urgency, frequency and incontinence are common coexisting complaints along with Pelvic floor dysfunction and possibly with constipation as well .The anterior vaginal wall supports the bladder and urethra.
When the prolapse is of a more severe degree P.O.P ,women complain of urinary hesitancy , intermittent flow , weak or prolonged stream , and also feeling difficulty with emptying or feeling the need to manually splint the prolapse to urinate.Possibly changing the sitting position on the toilet to facilitate completion or to start urination.
- Symptoms of moderate and severe degree are usually worse at the end of the day or with standing and exercises and improve with laying down .
- Prolapse symptoms primarily impact the quality of life and symptoms are not “dangerous” to life or medically but symptoms gradually and usually progressively get worse.Prolapse generally does not heal itself.
- Symptoms are usually better in gravity eliminated positions
- Symptoms more prominent with straining ..

Treatment for Prolapse:
Conservative Treatment:
- “Wait and Watch”(depending on the degree of prolapse)
- Pessary
- Physical Therapy.
Surgical Repair of Prolapse :Surgical repair of prolapse is performed by a Urogynecologist.

What can one expect when seen by the Dr.(Urogynecologist)
- The Dr would examine the symptoms to evaluate the degree of organ prolapse based on the prolapse grading system.
- A vaginal exam will be performed and the patient asked to strain to produce the maximum extent of prolapse.Various instruments may be used.
- Depending on the degree of prolapse and if weakness is found in the pelvic floor muscles, the patient may be referred to the pelvic floor therapist. A pelvic floor therapist is a physical therapist who undergoes additional specialised training and board testing to treat patients with issues of the pelvic region related diagnosis.
- When appropriate the patient may be fitted with a Pessary.
Pessary:
- A Pessary is an intravaginal device used to support the vaginal wall in women with P.O.P.
- A Pessary is generally prescribed by the urogynecologist and they are made in various shapes and sizes.
- They are mostly made of silicone.
- Pessary is used as a safe alternative to surgery when appropriate.
- There has been no high-level research based evidence of the effectiveness of pessaries to manage P.O.P.
- Pessary seems to be effective in improving the pelvic floor symptoms as evidenced by clinical trials that showed significant symptom relief and improvement in the quality of life, satisfaction and sexual function.
- Women fitted with pessaries are advised to remove and reinsert periodically to avoid complications of pessary use like, vaginal bleeding erosion and infection.Regular follow up with Dr. is recommended.

Physical Therapy and Prolapse :
- Women cannot change their genetic predisposition but can certainly do what can be done what is in their control which is exercise. Pelvic floor muscle strengthening exercises, Kegels have been proven to help prevent the symptoms and even to improve the symptoms of urinary urgency frequency if present.
- Regular Pelvic floor muscle strengthening helps to strengthen and retain the muscles and nerves of the Pelvis.
- Download my helpful instructions on Kegel Exercises.
- If you suspect you have prolapse or have any questions please comment or contact me via email .I will be happy to answer your questions or point you in the right direction, if possible .


Resources :
Association for Pelvic organ Prolapse Support (APOPS)
Private Facebook Groups for Pelvic organ Prolapse
References :
Evidence-based Physical Therapy for Pelvic floor 2nd Edition.
Pelvic Floor Dysfunction and Treatment , Level 1 Herman and Wallace Pelvic Rehabilitation Institute
Declancy,J.O. 1994 Structural support of urethra as it relates to stress incontinence, the hammock hypothesis .AM. J .Obstet. Gynecol. 170 ,1713 to 1720
